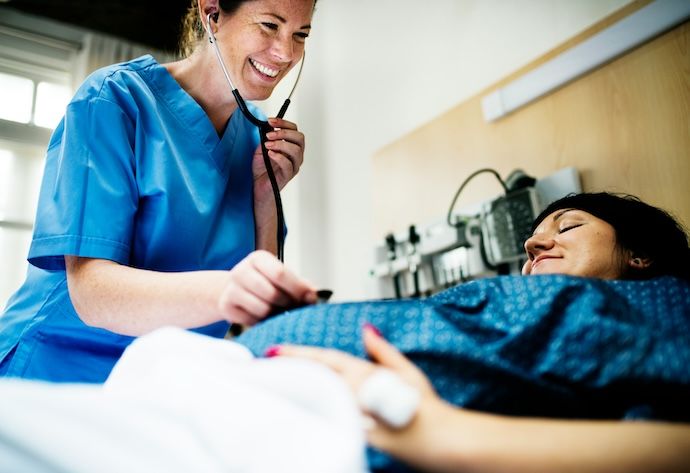
Midwives Burnout: Toxic Cycle of Staff Shortages and Resignations
One midwife, who doesn't want to be identified, has just handed in her notice after nine years in the role. She cites the demoralizing effects of the maternity sector as the key reason for her decision. Midwives are leaving the profession in droves, exhausted by burnout and rising pressure.
Midwifery Councils say the current staffing crisis in the profession is "unsustainable". Midwives are struggling to cope with an ever-increasing workload as hospitals cut back on staff and funding. This has resulted in a vicious cycle of resignations and further pressure on those who remain. One midwife, who doesn't want to be identified, has just handed in her notice after nine years in the role. She cites the demoralizing effects of the maternity sector as the key reason for her decision. "The whole thing has become a soul-destroying experience," she says. "I can't tell you how many times I've been reduced to tears by the things that have happened in my job."
She points to ever-increasing pressure on midwives and a lack of appreciation from management as key reasons for her departure. "It feels like we're constantly being asked to do more with less," she says. "And when things go wrong, it's always us who are blamed.
An urgent review of staffing levels and funding for the profession is needed. In the meantime, councils are urging midwives to take care of their own well-being and to seek support if they are struggling. The MIdwifery Council point out that midwives are being "pushed to breaking point". It is time for action to be taken to address the staffing crisis in the profession. Midwives deserve better working conditions, pay, and support. We cannot continue to lose them to burnout.
This toxic cycle affect patients
The most obvious way that patients are affected by this toxic cycle is through the increased pressure it puts on remaining staff members. This can lead to sub-standard care, as midwives simply don't have the time or energy to provide the level of service that they ideally would like to. In some cases, it can even lead to dangerous situations, as exhausted midwives make mistakes that could put mothers and babies at risk.

Photo by Claudia Wolff on Unsplash
It's not just the quality of care that suffers though; patients also face longer wait times and reduced access to services due to staffing shortages. Midwives are often forced to prioritize emergency cases over routine appointments, meaning that pregnant women who just need a check-up may have to wait weeks or even months to see someone. This can be extremely stressful for expectant mothers, who may already be anxious about their pregnancy.
In some cases, the staffing shortages are so severe that hospitals are forced to close their doors to new patients altogether. This means that women who have just gone into labor may have to travel long distances to find a facility that has the capacity to take them in. The journey itself can be dangerous for both mother and child, and it adds an extra layer of stress to an already difficult situation.
The toxic cycle of staff shortages and resignations is having a serious impact on patients. Midwives are working themselves to the point of exhaustion, and it's simply not sustainable in the long run.
Different solutions are needed to address the issue
There is no one-size-fits-all solution to addressing the issue of midwife burnout, but there are some steps that can be taken to try and mitigate the problem.
One way to address the issue is by ensuring that midwives have access to adequate support systems. This could include things like having more experienced midwives on hand to provide guidance and support to newer staff, as well as making sure that there are adequate counselling and mental health services available for midwives who are struggling with the demands of their job.
Another way to try and reduce the incidence of burnout amongst midwives is by improving working conditions. This could involve things like increasing staffing levels so thatmidwives are not overworked, as well as ensuring that they have access to proper breaks and rest periods.
Ultimately, addressing the issue of midwife burnout will require a multifaceted approach. By taking steps to improve working conditions and support systems, we can start to make a difference for the women who dedicate their lives to this vital profession.
Midwives are some of the most hardworking and dedicated professionals in our society. They play a vital role in bringing new life into the world, and yet they are often undervalued and overworked. The problem of midwife burnout is one that needs to be addressed urgently if we want to protect the health of both mothers and babies.
Midwifery staff shortages are a global problem
With over 55% of WHO Member States reporting to have less than 40 nursing and midwifery personnel per 10 000 population, the World Health Organization estimated 2021 a shortfall of nearly 900,000 midwives.
In the UK, The Health and Social Care Committee’s Expert Panel found '...that 8 out of 10 midwives reported that they did not believe that there were enough staff on their shift to be able to provide a safe service and every unit has rota gaps for doctors'. The Royal College of Midwives (RCM) has warned that the number of midwives in England dropped by 552 midwives from 05/2021 to 05/2022 coupled with an existing shortage of over 2,000 midwives.
Maternity services are under immense pressure with an increase in the birth rate, more women with complex needs and an ageing midwifery workforce. Midwives are working excessive hours often taking work home with them and feeling unable to provide the high standard of care they want to.
New Zealand is not immune to this global problem. A survey of Midwifery employees (n=573) found that 60% reported symptoms of anxiety and 45% depression. Midwives in New Zealand are leaving their jobs in droves, according to new statistics from the country’s health ministry. The number of midwives who resigned or left their positions voluntarily in 2017 was nearly 50% higher than the number who did so in 2012. Officials say they expect the trend to continue, with 2022 being the year that most midwives will have left their jobs.
The health ministry has put forth a number of possible explanations for the exodus, including poor working conditions and a lack of professional development opportunities. Midwives in New Zealand are also paid relatively poorly compared to those in other developed countries, which may be contributing to the problem.
Officials say they are taking steps to address the issue, but they admit that it may be difficult to retain midwives without offering them better pay and working conditions.
There is a real crisis in midwifery with staff shortages, excessive workloads and low morale. This toxic cycle needs to be broken before we lose even more midwives to burnout and resignation.
With countries like Australia and New Zealand also struggling to keep up with demand. In the UK, the Royal College of Midwives (RCM) has called on the government to invest more in midwifery services, warning that without urgent action "lives will be put at risk". It's time for action to address this critical issue. Otherwise, we'll continue to see an exodus of experienced midwives, and even greater pressure on those who remain.
A study by the Midwifery Taskforce in 2020 found that one in three newly qualified midwives were considering leaving the profession within five years and a survey of UK midwives found that over 70% had considered quitting due to stress and workload.
Burnout among health-care workers has been declared a public health crisis by the World Health Organization. In a global survey of over 130,000 health-care workers, 34% reported symptoms of burnout.
Conclusion
There are a number of reasons for midwife burnout: long hours, working weekends and holidays, being on-call 24/seven, being responsible for the safety of mothers and babies, shift work, understaffing and lack of support. Midwives are also more likely to experience vicarious trauma or compassion fatigue due to the nature of their job.
The effects of burnout go beyond the individual midwife. Midwife burnout can have a negative impact on retention rates, patient safety and quality of care. A study in the USA found that nurses who were experiencing high levels of burnout were more likely to make errors in patient care.
Burned-out midwives are more likely to leave the profession, exacerbating the already critical staff shortages. The high levels of stress and burnout among midwives is having a negative impact on their mental and physical health, as well as their personal lives. Midwives have reported feeling depressed, anxious and stressed, and many say they are struggling to cope. Some have even been diagnosed with post-traumatic stress disorder (PTSD).